Precision microbiome engineering study: "The level of control and precision of engraftment that we have achieved is unprecedented"
A new study from Prolacta Bioscience recently published a report that demonstrated that human milk oligosaccharides (HMOs) and Bifidobacterium infantis can safely and predictably control the gut microbiome in adults.
The research, published in Cell Host & Microbe, illustrates scientists’ ability to modulate the adult gut microbiome with significant precision.
Gregory McKenzie, PhD, VP of Product Innovation at Prolacta Bioscience and co-author of the current study, told NutraIngredients-USA that the prospect of precision microbiome engineering may open the door to the development of live biotherapeutic products to improve outcomes in numerous patient populations.
“Current methods for modulating the microbiome are either to take antibiotics, that indiscriminately kill many of the microbes in our guts, or to take a cocktail of microbes (via fecal transplant) and hope that some of those microbes engraft and do some of the jobs that our microbiome is supposed to do. Our human milk-based synbiotic allows us to deliver a microbe (B. infantis) that is a normal, healthy resident of the nursing infant gut, and to control how it engrafts. And when we stop treatment, we can cause B. infantis to go away. The level of control and precision of engraftment that we have achieved is unprecedented,” said McKenzie.
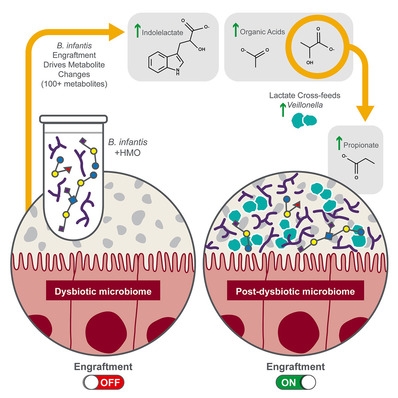
He added that B. infantis engraftment causes the production of a variety of molecules that are beneficial to patients, including short-chain fatty acids and indoles, both of which play roles in the development of a healthy immune system and in ensuring gut barrier integrity.
The study
Researchers from Prolacta, MD Anderson Cancer Center and the University of Texas Southwestern Medical Center observed that HMOs support engraftment of B. infantis in healthy adults with a median abundance of about 46% and up to 81% relative abundance in antibiotic-treated adults.
The report also noted that microbiome structure and gut metabolite levels were altered in engrafted subjects. When B. infantis was present, other members of the microbiome that are not directly influenced by HMOs changed in a reproducible manner. For example, there is a microbe called Veillonella that feeds on molecules produced by B. infantis and subsequently generates metabolites that are beneficial to human health.
“The reproducibility of cross-feeding Veillonella is really striking, as this magnitude of downstream effects are normally seen only when treating patients with antibiotics,” said first author Julie Button, PhD, director, non-clinical development at Prolacta.
The results suggest that the synbiotic reproducibly and predictably modulates recovery of a dysbiotic microbiome.
“We are demonstrating that the same biology that develops a healthy infant gut can be applied to adults with disrupted gut microbiomes. This is tremendously exciting. We can leverage our understanding of how babies are naturally protected from infection and inflammatory disease, and start to have an impact on adult patients with infectious and inflammatory diseases,” said McKenzie.
While our next clinical trial is in adults undergoing allogeneic stem cell transplants, we expect that this synbiotic will be applicable to a broad variety of infectious, autoimmune, and metabolic disorders.”
Coming up
“We expect that this human milk-based synbiotic will have the power to repair the microbiome of sick patients using the same biology that establishes a healthy microbiome in infants,” said Scott Elster, CEO of Prolacta. “We plan to demonstrate what is essentially `Nature’s Microbiome Starter Kit’ in extremely fragile stem cell transplant patients in a Phase 2a clinical trial starting in Q3 2023.”
Source: Cell Host & Microbe
doi.org/10.1016/j.chom.2023.08.004
Precision modulation of dysbiotic adult microbiomes with a human-milk-derived synbiotic reshapes gut microbial composition and metabolites
Authors: J Button, et al.