Vitamin D in the US: ‘Those with greatest need of dietary sources of vitamin D have the lowest intakes’
While 60% of vitamin D intakes in Canada and the US come from fortified foods like milk, low consumption of such products by key sections of the population means that alternative ways of delivering the sunshine vitamin are needed, wrote FDA’s Mona Calvo and Saskatchewan’s Susan Whiting.
Writing in The Journal of Steroid Biochemistry and Molecular Biology, Calvo and Whiting note that ‘bio-addition’ may “provide a wider range of foods containing vitamin D, and thus appeal to differing preferences, cultures and possibly economic status”.
‘Bio-addition’ refers to the addition of vitamin D-rich food to animal feed during production, or manipulation of food post-harvest or pre-processing. Such approaches include exposure edible mushrooms to UV light.
The vitamin
Vitamin D refers to two biologically inactive precursors - D3, also known as cholecalciferol, and D2, also known as ergocalciferol. The former, produced in the skin on exposure to UVB radiation (290 to 320 nm), is said to be more bioactive.
Both D3 and D2 precursors are hydroxylated in the liver and kidneys to form 25- hydroxyvitamin D (25(OH)D), the non-active 'storage' form, and 1,25-dihydroxyvitamin D (1,25(OH)2D), the biologically active form that is tightly controlled by the body.
While our bodies do manufacture vitamin D on exposure to sunshine (UV-B radiation with a wavelength between 290 and 315 nm), the levels in some northern countries are so weak during the winter months that our body makes no vitamin D at all, meaning that dietary supplements and fortified foods are seen by many as the best way to boost intakes of vitamin D.
Inadequacy and deficiency
Despite the opportunities to enhance vitamin D intakes via food and supplements, many sections of the population are still not getting enough, said Calvo and Whiting.
Data from both countries showed that whites had the highest vitamin D levels, followed by Hispanics. African Americans had the lowest average levels.
“Those in greatest need of dietary sources of vitamin D have the lowest intakes of vitamin D, on top of a reduced potential for adequate sun-induced synthesis of vitamin D,” wrote the researchers.
“Neither country has population mean intakes that meet current estimated average requirement (EAR) level of 400 IU.”
Solutions
A number of foods are allowed to be fortified with the vitamin, including fluid milk, soy beverage products, ready-to-eat breakfast cereal, enriched rice, calcium-fortified 100% fruit juice, enriched cornmeal products, yogurt, cheese and cheese products, meal replacements, margarine, and infant formula.
In addition, ‘bio-addition’ may help increase consumption among sections of the populations that do not currently consume some of these food because of food preferences, cultural tastes, and costs, said Calvo and Whiting.
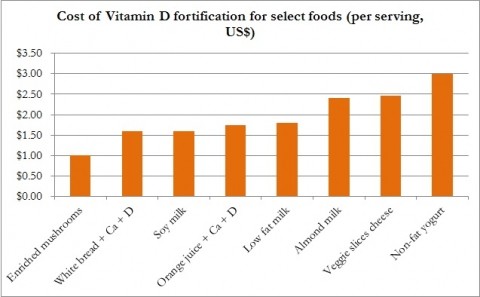
Costs associated with fortifying select foods are shown in the graph below.
Take home
“In Canada and the United States, the adequacy of foods fortified with vitamin D to meet the needs of all race, gender and age groups has been called into question,” wrote Calvo and Whiting.
“Much of the intake of vitamin D from foods in the United States and Canada is from fortified foods.
“Fortification practices are different between USA and Canada, the former having a voluntary approach and the latter stressing mandatory fortification; nevertheless both are similar in providing fortified foods with proven efficacy, but more needs to be done.”
Source: The Journal of Steroid Biochemistry and Molecular Biology
Published online ahead of print, doi: 10.1016/j.jsbmb.2012.09.034
"Survey of current vitamin D food fortification practices in the United States and Canada"
Authors: M.S. Calvo, S.J. Whiting